Stress, Flares, and the Nervous System: Why Lichen Sclerosus Worsens Without Visible Triggers

One of the most confusing moments in lichen sclerosus is this:
You’re doing everything “right.”
Treatment is consistent.
Products are gentle.
The skin looks calm.
And yet symptoms rise anyway.
Burning increases.
Sensitivity spikes.
Pain appears without a clear trigger.
This is where many people start blaming themselves or assuming the disease is “progressing.”
My view is different and very clear:
many LS flares are not driven by visible skin damage, but by nervous system and stress related immune signaling.
If this layer is ignored, flares feel random and uncontrollable.
Why Stress Affects LS Even When the Skin Looks Calm
Stress is not just emotional.
It directly affects:
- immune signaling
- nerve sensitivity
- skin blood flow
- inflammatory thresholds
In lichen sclerosus, these systems are already sensitized.
Stress does not need to be extreme.
Chronic, low grade stress is enough to lower the threshold at which symptoms appear.
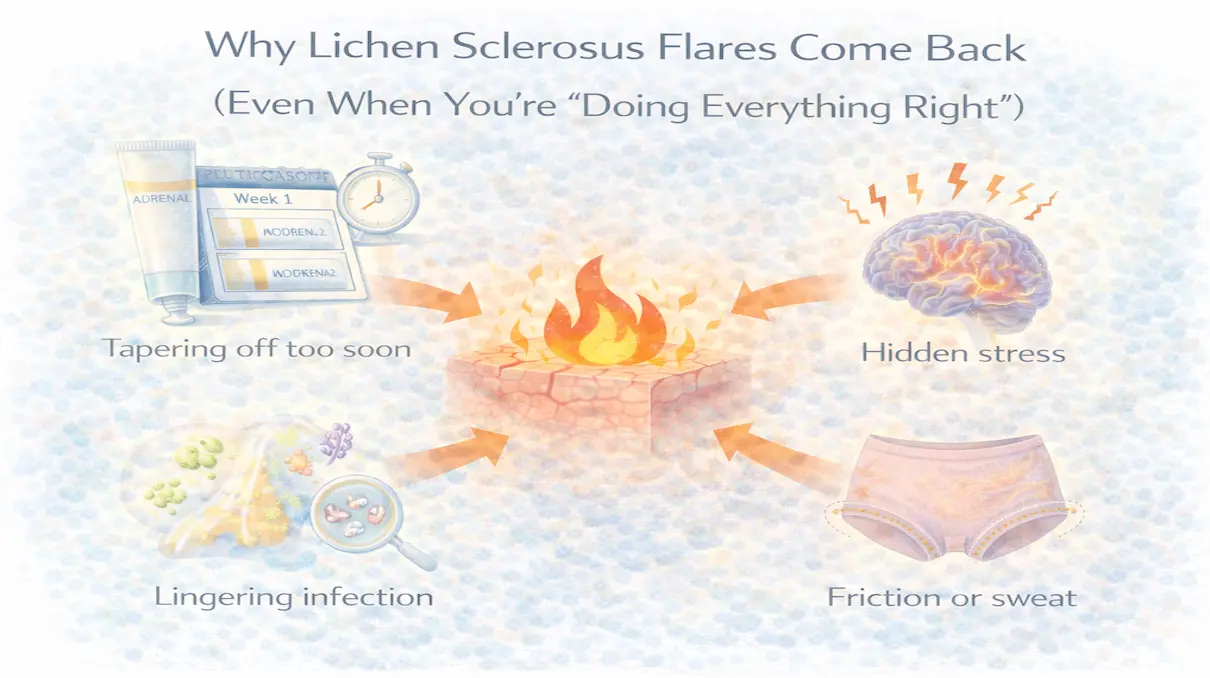
That’s why flares can happen without:
- new products
- obvious friction
- infection
- treatment failure
The trigger is internal not imaginary.
The Skin Nervous System Connection (The Missing Explanation)
The skin is one of the most densely innervated organs in the body.
It constantly communicates with:
- peripheral nerves
- immune cells
- the brain
During stress, several biological changes occur simultaneously:
- nerves become more reactive
- mast cells degranulate more easily
- cytokines such as IL-6 and TNF-α increase
- blood flow patterns shift
These changes can produce:
- burning
- itching
- tightness
- hypersensitivity
without visible inflammation or tissue damage.
Why Stress Related Flares Feel “Different”
People often describe stress driven flares as:
- burning without redness
- diffuse soreness
- increased awareness of the area
- symptoms that fluctuate hour to hour
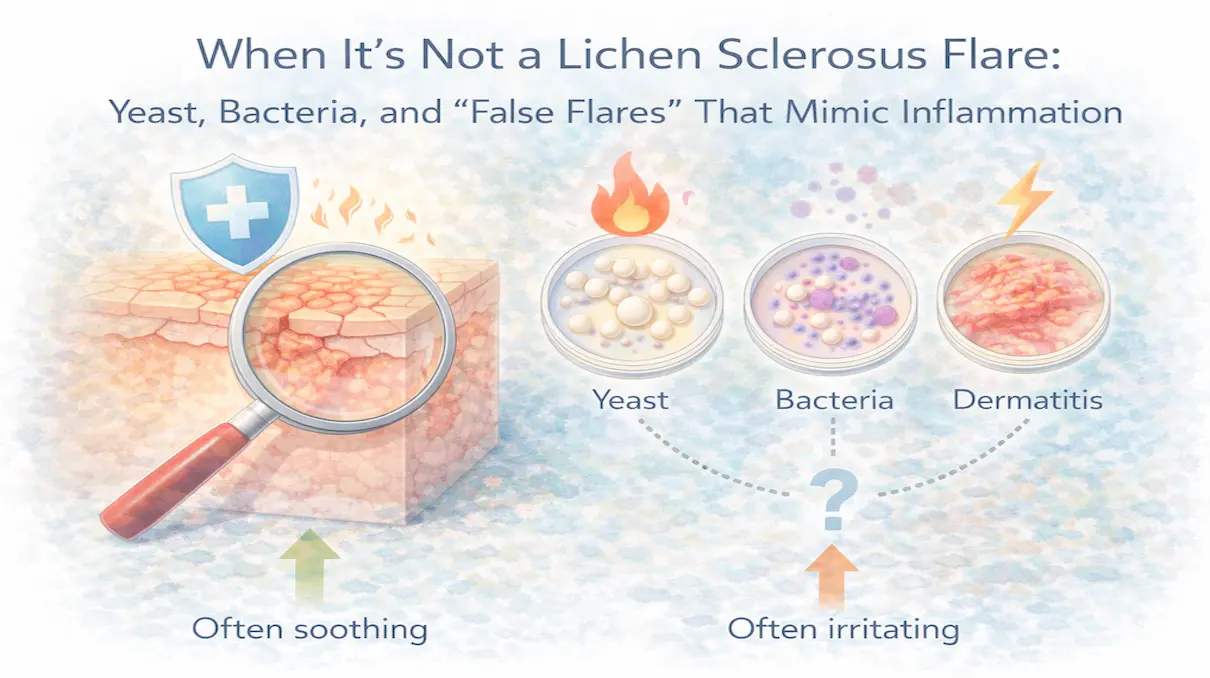
Unlike classic inflammatory flares, these may:
- respond poorly to escalating steroids
- improve unpredictably
- worsen with monitoring or worry
This doesn’t mean inflammation is absent.
It means neuro immune signaling is dominant.
Cortisol, Adrenaline, and Immune Dysregulation
Stress triggers the release of cortisol and adrenaline.
Short term:
- cortisol is anti inflammatory
Long-term stress:
- dysregulates immune responses
- increases mast cell sensitivity
- lowers flare thresholds
- impairs resolution of minor triggers
In LS, this keeps the skin in a “ready to react” state, even when nothing obvious is wrong.
Why “Nothing Changed” Is Often the Clue
When people say:
“I didn’t change anything, it just got worse”
That often points toward:
- cumulative stress
- nervous system overload
- lack of recovery time
Stress driven flares are rarely about a single event.
They’re about load, not mistakes.
The Role of Attention and Monitoring (Without Blame)
This is delicate but important.
Constantly checking symptoms:
- increases nervous system arousal
- amplifies pain perception
- reinforces threat signaling
This does not mean symptoms are imagined.
It means attention can intensify real biological sensations.
Many people notice improvement when they:
- stop checking constantly
- reduce health related anxiety
- stabilize routines instead of optimizing endlessly
This is nervous system biology, not denial.
Stress, Daily Care, and the Over Treatment Trap
Stress often pushes people toward:
- overwashing
- overtreating
- product hopping
- constant adjustments
These behaviors increase:
- friction
- chemical exposure
- barrier disruption
Which reinforces symptoms and stress.
Ironically, doing more is often the flare trigger.
Why Barrier Care Still Matters During Stress Flares
Even when stress is the main driver, barrier care remains critical.
Stable, boring protection reduces:
- friction induced nerve firing
- mechanical retriggering
- sensory overload
This is why people often stabilize when they rely consistently on:
- petrolatum / Vaseline for friction reduction
- Cicalfate when skin feels raw or reactive
- Cicaplast B5+ during stable phases
- VEA Lipogel, Vitamono EF, or zinc-based barriers for neutral daily protection
Barrier care doesn’t treat stress,
it prevents stress from becoming skin inflammation.
The Stress Pain Inflammation Loop
Stress increases nerve sensitivity.
Sensitive nerves amplify discomfort.
Discomfort increases stress.
This loop can persist even when:
- the original trigger is gone
- inflammation is medically controlled
- the skin looks normal
Breaking the loop requires calming both the skin and the nervous system.
Why “Relax More” Is the Wrong Advice
Being told to “relax” is unhelpful.
What actually helps is:
- understanding why stress affects symptoms
- reducing unpredictability in routines
- minimizing decision fatigue around care
- restoring a sense of control
The nervous system calms when life feels structured and predictable, not when pressure is added.
When Stress Is Likely the Main Driver
Stress is often a dominant factor when:
- flares coincide with emotional strain
- symptoms fluctuate rapidly
- pain feels disproportionate to skin changes
- treatment response becomes inconsistent
- fear dominates daily decisions
Recognizing this shifts the strategy from escalation to stabilization.
When Medical Reassessment Is Still Important
Stress does not explain everything.
Medical review is essential if:
- skin changes progress
- symptoms steadily worsen
- new lesions appear
- pain becomes severe or disabling
Stress and inflammation often coexist, addressing one does not replace treating the other.
A Healthier Mental Model
Instead of asking:
“What did I do wrong?”
Ask:
“Which system is reacting right now: skin, nerves, or both?”
That question reduces panic and leads to better decisions.
Final Thought
Lichen sclerosus does not live only in the skin.
It lives at the intersection of:
- immune signaling
- nerve sensitivity
- mechanical stress
- emotional load
When stress and the nervous system are addressed alongside medical treatment, flares become less frequent, recovery is faster, and life feels more manageable.
Calming the nervous system is not a replacement for medical care,
it’s often the missing layer that allows care to work.