Do I Have Lichen Sclerosus? A Complete Guide to Symptoms, Diagnosis, and What It Gets Mistaken For

Do I Have Lichen Sclerosus? A Complete Guide to Symptoms, Diagnosis, and What It Gets Mistaken For
You noticed something was wrong. Maybe it started as itching, the kind that comes at night and doesn't quite stop. Maybe you spotted a change in the skin: a pale patch, a small tear, a persistent soreness that never fully resolved. You searched online, asked a doctor, and somewhere along the way the words lichen sclerosus appeared. Or maybe they haven't yet, and you're here trying to figure out whether that's what this is.
Either way, you're in the right place.
Lichen sclerosus is frequently misdiagnosed, often for years. It gets called a yeast infection. Contact dermatitis. Atrophy. Stress. By the time many patients receive a correct diagnosis, they've tried several treatments that didn't work, because they were treating the wrong thing.
This guide covers what lichen sclerosus actually looks and feels like, how it gets confused with other conditions, how it's properly diagnosed, and what to do once you have a confirmed diagnosis.
What is lichen sclerosus, in plain terms?
Lichen sclerosus (LS) is a chronic inflammatory skin condition that primarily affects the vulva in women, though it can also occur on the penis, anus, and very rarely on other skin surfaces. It's not contagious, not caused by poor hygiene, and not the result of anything you did wrong.
The disease involves the immune system mistakenly targeting skin tissue, leading to inflammation, structural changes, and loss of tissue elasticity over time. It tends to be cyclical, periods of active symptoms alternating with quieter phases, which is part of why it can feel so unpredictable.
It's more common than most people realize. Estimates suggest it affects roughly 1 in 80 women, with peak onset around menopause, though it can appear at any age, including in children.
What makes lichen sclerosus particularly tricky is that its symptoms overlap significantly with other conditions. That overlap is responsible for most of the diagnostic delays patients experience.
The main symptoms of lichen sclerosus
Symptoms vary between patients and can change over time depending on what stage the disease is in. Some people experience all of the following. Others experience only one or two, intermittently.
Itching, often the first and most persistent symptom
The itch of lichen sclerosus has a particular quality that many patients describe as deep, relentless, and worse at night. It's not the surface level itch of a rash. It often feels like it comes from inside the tissue. Scratching brings only brief relief, and can make things significantly worse by damaging already fragile skin.
Not everyone with LS has severe itching. Some patients have very little itch but significant burning or structural changes. Absence of itch does not rule out the diagnosis.
Burning and stinging
Burning is often described as the second most disruptive symptom. It can occur during urination, sex, or simply from contact with clothing. The burning may be constant during flares or appear specifically after friction or moisture exposure.
Pain, including pain during sex
Dyspareunia (painful intercourse) is one of the symptoms that brings many patients to seek diagnosis. The skin of the vulva in LS often becomes fragile and less elastic, making penetration painful or impossible during active phases. This symptom is frequently attributed to dryness, vaginismus, or psychological causes before LS is considered.
White patches and skin changes
The most visually distinctive sign of lichen sclerosus is white or ivory patches of skin, typically appearing on the vulvar area. These patches may have a crinkled, cigarette paper texture, especially in more advanced cases. The skin may look thin and fragile.
Importantly: white patches don't necessarily mean the disease is currently inflamed. They can reflect structural changes in the tissue that occurred during previous active phases. Some patients have significant white discoloration with minimal current symptoms. Others have intense symptoms with minimal visible change.
Skin tears, fissures, and erosions
When the skin barrier becomes fragile, small tears or fissures can appear, often at the posterior fourchette (the lower junction of the vaginal opening) or around the clitoris. These are painful, slow to heal, and can reopen with normal activities like walking or sitting.
Tightening and structural changes
Over time, without adequate management, LS can cause fibrotic remodeling, a progressive tightening of the tissue. The clitoral hood may fuse over the clitoris. The vaginal opening may narrow. The labia minora can partially disappear. These structural changes are what make early diagnosis and consistent treatment so important.
These changes don't happen quickly, and many can be slowed or stabilized with proper care. But they are not reversible once established, which is why waiting for symptoms to resolve on their own is not a safe approach.
Symptoms that appear without visible changes
One of the most disorienting experiences patients describe is persistent pain, burning, or sensitivity when the skin looks entirely normal, or nearly so. This happens because nerve pathways in affected tissue can remain sensitized even when visible inflammation has calmed. It's real, it's documented, and it's not in your head.
Worth noting: Lichen sclerosus does not behave identically in every person. Symptom severity, location, and pattern all vary. If your experience doesn't match a textbook description, that doesn't mean you don't have it.
What lichen sclerosus gets mistaken for
Diagnostic delays of two to five years are not uncommon. Here's why, and what conditions are most frequently confused with LS.
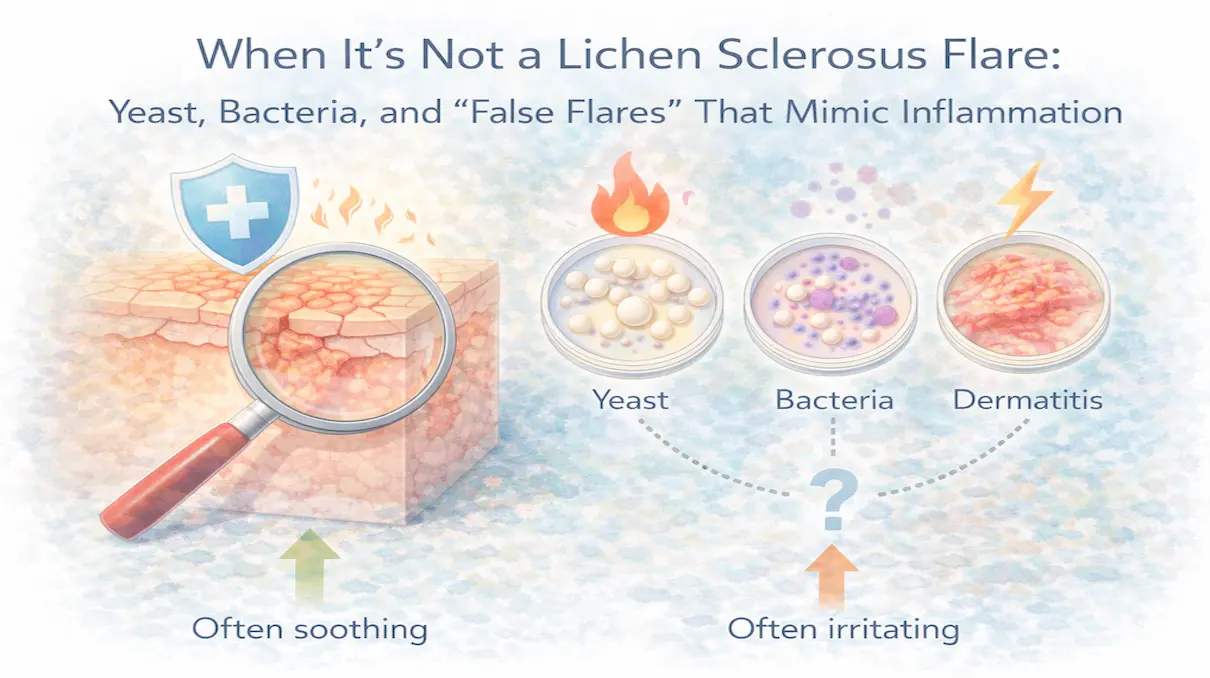
Yeast infections (candidiasis)
Itching and burning overlap almost perfectly between LS and recurrent yeast infections. Many patients treat themselves for yeast infections for months or years before seeking further investigation. The key difference: antifungal treatment resolves a yeast infection within days. If symptoms keep returning or never fully clear, yeast is not the whole story.
It's also worth knowing that LS patients are more vulnerable to secondary yeast infections, so both can be present at the same time. A positive yeast swab does not rule out LS.
Contact dermatitis
Irritant or allergic contact dermatitis from soaps, detergents, hygiene products, or topical medications can cause burning, redness, and itching that looks similar to an LS flare. The distinction matters because some patients with LS have concurrent contact sensitivities, and those sensitivities can trigger or worsen LS symptoms.
If patch testing reveals a contact allergy, eliminating the trigger often dramatically reduces symptoms. But if the underlying LS isn't also addressed, the skin will remain vulnerable.
Related: LS vs Yeast vs Dermatitis: Why Misdiagnosis Is Common
Lichen planus
Lichen planus is a different inflammatory skin condition that can affect similar areas. It tends to cause erosions and a lacy white pattern rather than the thickened white plaques of LS, and often involves the vaginal canal (which LS typically does not). The treatments overlap somewhat, but the distinction matters for long term management. A biopsy is usually needed to differentiate them reliably.
Vulvodynia
Vulvodynia is chronic vulvar pain without an identifiable cause. It often coexists with LS, and the two can be difficult to separate clinically. Patients with LS who continue to experience significant pain even when inflammation is controlled may have a concurrent vulvodynia component. Treatment for LS alone may not fully resolve pain in these cases.
Atrophic changes (GSM / menopause-related)
Genitourinary syndrome of menopause (GSM) causes thinning, dryness, and fragility of vulvovaginal tissue due to declining estrogen. The symptoms overlap significantly with LS, and both conditions can occur simultaneously in postmenopausal women. Treatment differs: GSM responds to topical estrogen, while LS requires a different approach entirely.
If you've been given topical estrogen for dryness and it hasn't resolved the problem, LS should be considered.
Psoriasis
Vulvar psoriasis presents with redness, itching, and discomfort. It typically does not cause white patches or the structural changes associated with LS, but in early stages or atypical presentations, the distinction isn't always obvious on clinical examination alone.
How lichen sclerosus is diagnosed
There is no blood test for lichen sclerosus. Diagnosis is primarily clinical, meaning it's based on examination, sometimes with biopsy confirmation.
Clinical examination
An experienced dermatologist or gynecologist can often diagnose LS on visual examination alone, particularly when characteristic white patches, tissue fragility, and architecture changes are present. The pattern and location of changes are often distinctive enough that biopsy isn't needed for a confident diagnosis.
However, clinical examination alone can miss early stage LS, atypical presentations, or cases where visible changes are subtle.
Skin biopsy
A biopsy is the gold standard for confirming the diagnosis, ruling out other conditions, and identifying precancerous changes. A small piece of tissue is taken under local anaesthetic and examined microscopically. It typically reveals a characteristic pattern: epidermal thinning, loss of the rete ridges, and a band of inflammatory cells and fibrotic change in the upper dermis.
A biopsy is recommended when:
- the diagnosis is uncertain after examination
- symptoms haven't responded as expected to treatment
- a lesion looks unusual or has changed in appearance
- malignant transformation needs to be ruled out
Biopsy is not painful beyond the anaesthetic injection and heals quickly. If you've been managing symptoms for a long time without a confirmed diagnosis, requesting a biopsy is reasonable.
Dermoscopy
Dermoscopy, a magnified examination of the skin surface, is increasingly used by dermatologists to visualize patterns associated with LS before biopsy. It can provide additional information and support clinical diagnosis in experienced hands.
Supporting tests
LS is associated with other autoimmune conditions, particularly thyroid disease. Once LS is diagnosed, many clinicians recommend checking thyroid function and thyroid antibodies. This isn't part of the diagnostic process itself, but it's clinically useful information.
Hormonal testing, allergy patch testing, and vitamin D levels may also be relevant depending on your symptoms and presentation. These won't diagnose LS, but they can identify contributing factors worth addressing.
If you're asking: Do I need a biopsy to start treatment? Not necessarily. If the clinical picture is clear, most doctors will begin treatment without waiting for biopsy results. But a confirmed diagnosis is always better than an assumed one.
What to do if you suspect lichen sclerosus
If you recognize your symptoms in what you've read here, the next step is a proper evaluation. That means seeing someone who has experience with LS, ideally a dermatologist or a vulvar specialist rather than a general practitioner alone.
Before your appointment, it helps to:
- note how long you've had symptoms and how they've changed
- list every product you use in the affected area: soaps, wipes, lubricants, pads, laundry detergents
- note any patterns: does it worsen at a particular time of the month? after sex? after exercise?
- bring a list of any treatments you've tried and whether they helped
If you've already seen multiple doctors without a diagnosis, you are not being dramatic. You may simply need to see someone with more specific experience with this condition. A referral to a vulvar disease clinic or a dermatologist with a special interest in genital skin is often the right next step.
After diagnosis: what comes next
A diagnosis of lichen sclerosus is not a life sentence of suffering. Many people, with appropriate treatment and management, achieve long periods of stability and good quality of life.
The standard first line treatment is a potent topical corticosteroid, usually clobetasol propionate. It reduces inflammation effectively and is the most studied intervention for LS. For many patients, it provides significant relief.
What's equally important to understand is that LS involves more than inflammation alone. The skin barrier, nerve sensitivity, fibrotic changes, and environmental triggers all interact with the disease. Steroid treatment addresses the inflammatory component well, but a complete approach considers all these layers together.
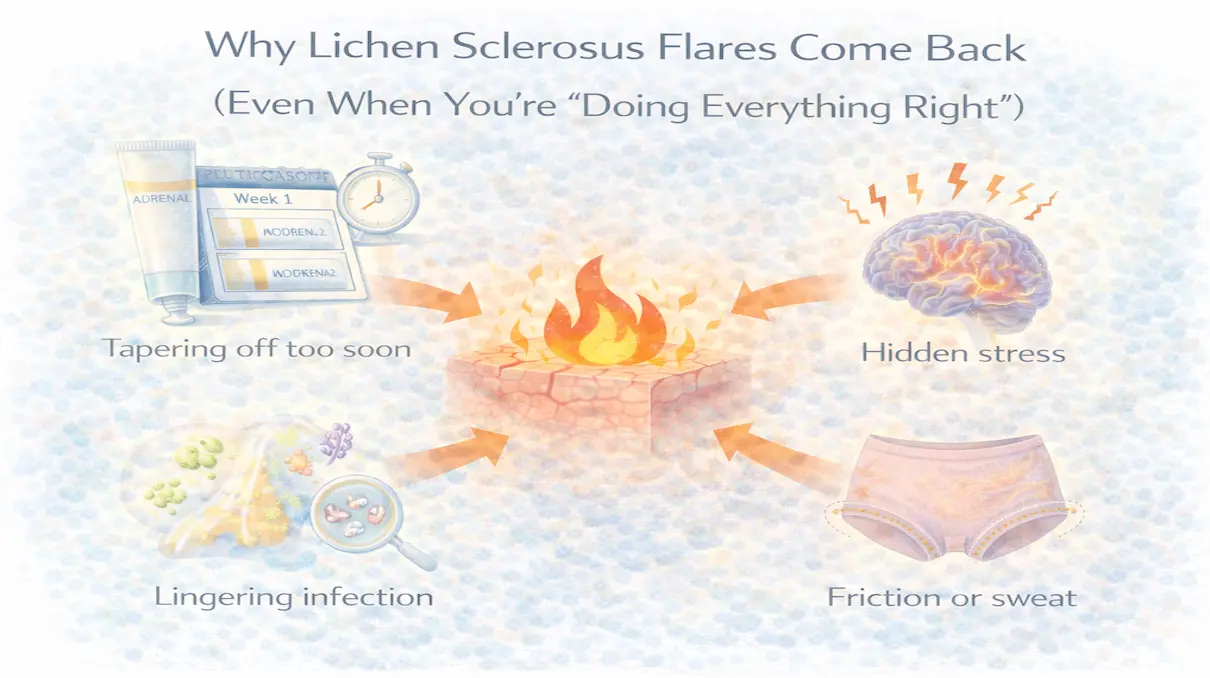
The disease also moves through phases. Knowing which phase you're in helps explain why some treatments feel more useful at certain moments than others, and why treatment that worked before can seem to stop working without warning.
Related: Can Lichen Sclerosus Go Into Remission? What the Evidence Says
Related: Why Steroids "Stop Working" in Lichen Sclerosus (And What's Actually Happening)
Related: Daily Care for Lichen Sclerosus: What Helps vs What Makes It Worse
A note on cancer risk
Lichen sclerosus does carry a slightly increased lifetime risk of vulvar squamous cell carcinoma, the most commonly associated skin cancer. The absolute risk remains low: the majority of LS patients never develop cancer.
But this is why untreated, poorly managed LS is a concern. Long term inflammation increases the likelihood of cellular changes over time. Consistent treatment, regular monitoring, and not ignoring unusual changes are the most important protective measures.
Changes that warrant prompt evaluation include: a sore that doesn't heal within two to three weeks despite proper care, a raised or thickened lesion that continues to grow, spontaneous bleeding from intact skin, or any change that looks distinctly different from your usual LS pattern.
None of this is meant to create anxiety. It's meant to underscore that lichen sclerosus is a condition that rewards attention, and that the patients who do best are the ones who understand their disease well enough to recognize when something has changed.
The bottom line
Lichen sclerosus is underdiagnosed, frequently misidentified, and often inadequately explained to the people who have it. If you've been living with unexplained vulvar symptoms: itching, burning, pain, fragile skin, white patches and haven't received a satisfying diagnosis, LS belongs on the list of possibilities.
A proper examination, and in many cases a biopsy, can give you a definitive answer. That answer is the foundation everything else is built on. Treatment without a correct diagnosis is, at best, guesswork.
If you do have lichen sclerosus: you're not alone, the condition is manageable, and understanding it clearly is the first step toward managing it well.
Content sourced from: Lichen Sclerosus Decoded, A New Way to Understand and Manage Lichen Sclerosus. For informational purposes only. This article does not constitute medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.