The Complete Lichen Sclerosus Trigger Guide: Why Flares Happen, What Causes Them, and How to Break the Cycle
The Complete Lichen Sclerosus Trigger Guide: Why Flares Happen, What Causes Them, and How to Break the Cycle
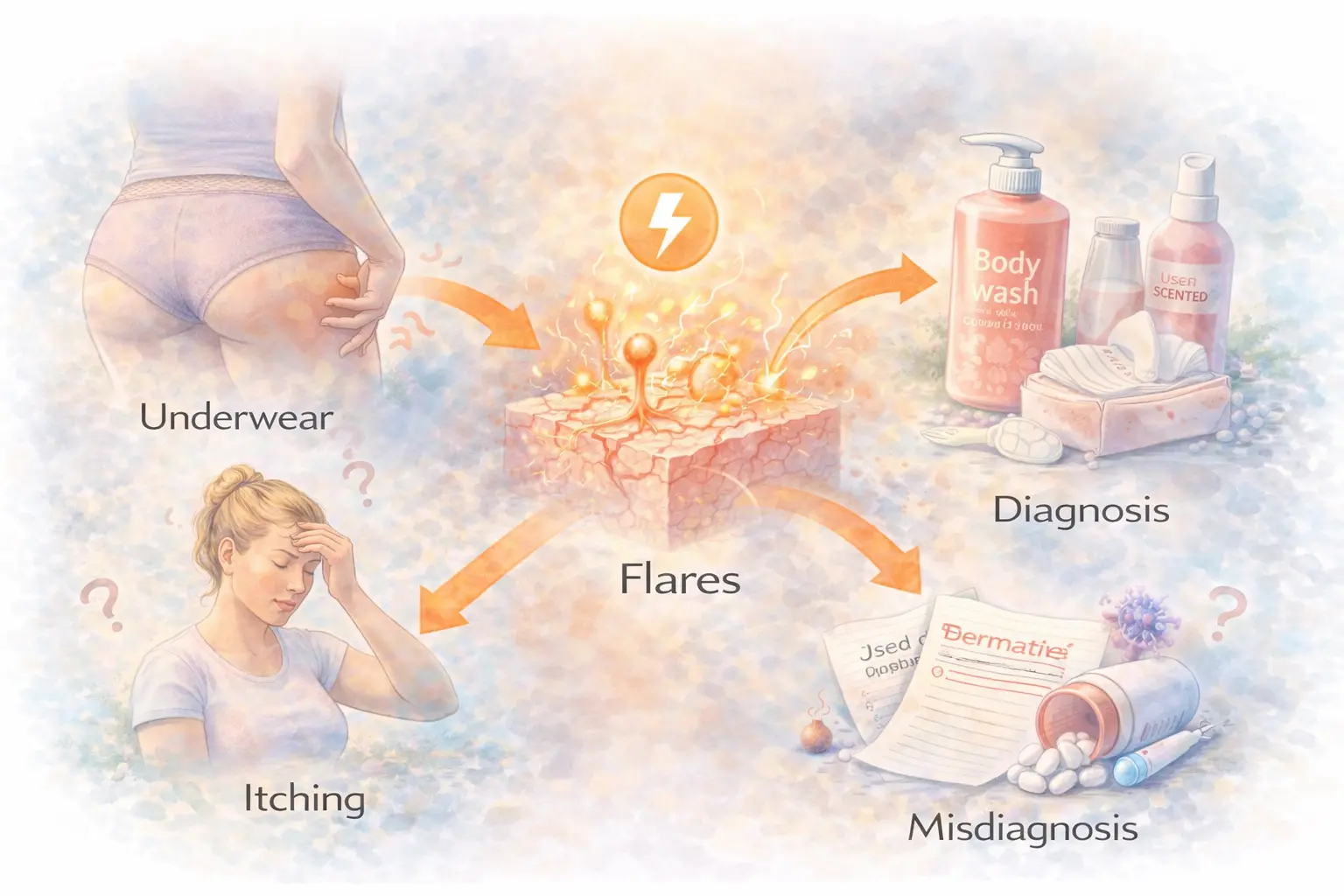
Here's something most patients figure out eventually, usually after months of frustration: lichen sclerosus flares are rarely random. They feel random. But when you look closely, really closely, over weeks of paying attention, a pattern almost always emerges.
Something happened before the flare. Maybe it was a new soap. A long bike ride. A stressful week. A course of antibiotics. The timing felt coincidental at the time, but it probably wasn't.
This is one of the most important shifts you can make in managing LS: from asking "why is this happening again?" to asking "what was different in the days before this started?" That second question is answerable. And the answer, once you find it, gives you something to work with.
This guide covers all seven major trigger categories, explains why the same trigger doesn't affect every patient equally, and gives you a practical framework for identifying your own personal pattern, because that's ultimately what matters most.
What a trigger actually is
A trigger is not a cause of lichen sclerosus. The disease is already there, driven by immune processes in the skin. A trigger is something that amplifies or reactivates those processes, that tips the skin from a state of relative stability into active inflammation or barrier breakdown.
Think of it this way: the skin of someone with LS is more easily provoked than normal skin. The threshold for irritation is lower. What a healthy person's skin shrugs off, a slightly rough fabric, a fragranced soap, a long walk can cross that threshold and set off a cascade.
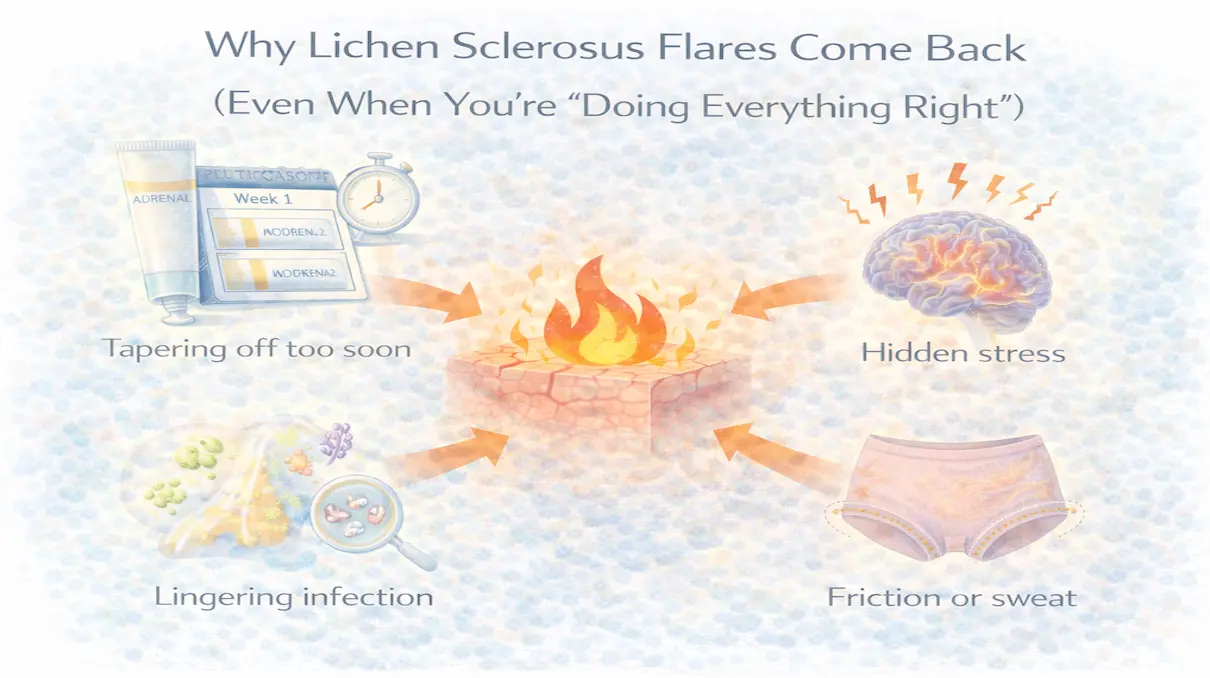
Once a flare begins, the immune system can amplify its own signals, which is why even a small trigger can sometimes produce a response that feels disproportionate. That amplification mechanism is covered in detail in the article on why lichen sclerosus flares keep coming back, what matters here is understanding that triggers are the spark, not the fire itself.
Related: Why Lichen Sclerosus Flares Come Back (Even When You're Doing Everything Right)
The practical implication: reducing triggers doesn't cure the disease, but it significantly lowers the frequency and intensity of flares. For many patients, trigger management is the intervention that makes the biggest visible difference to day to day quality of life.
The seven trigger categories
1. Mechanical friction
Friction is the most common and most underestimated trigger. The vulvar area experiences repeated physical stress throughout every ordinary day, from walking, sitting, clothing contact, exercise, and sexual activity. In normal skin, this causes no problem. In LS skin, where the barrier is already compromised, repeated friction can be enough to initiate inflammation.
The sources aren't always obvious. Tight waistbands. Seams in the wrong place. Synthetic fabrics that trap heat and moisture. Cycling or spinning classes. Long car journeys. Sitting on hard surfaces for hours. Sexual activity without sufficient lubrication. None of these feel damaging in the moment, and that's exactly why friction goes unrecognized for so long.
Hot weather makes friction worse because sweat increases the coefficient of friction between skin surfaces. Patients often notice a seasonal pattern, more flares in summer, without ever connecting it to this mechanism.
Related: Underwear, Fabrics, and Lichen Sclerosus: What Actually Makes a Difference
Related: Friction and Lichen Sclerosus: The Trigger Nobody Talks About
Related: Lichen Sclerosus and Daily Movement: How Walking, Sitting, and Exercise Affect the Skin
2. Chemical irritants
The vulvar skin is not the same as the skin on your forearm. It's thinner, more permeable, and far more reactive to chemicals. Products that are entirely harmless everywhere else on your body can cause significant irritation here.
The usual suspects: fragranced soaps and shower gels, feminine hygiene washes (including ones marketed as pH balanced or gentle), wet wipes, scented panty liners, bubble baths, bath bombs, fabric softeners, and laundry detergents. Even some prescription topical treatments can cause irritation in sensitive patients, if a cream burns consistently, that's information worth taking seriously.
The mechanism is primarily barrier disruption. Surfactants strip protective lipids from the skin surface. Fragrances cause direct inflammatory reactions in sensitized tissue. Preservatives can trigger contact allergies. Once the barrier is disrupted even slightly, the skin becomes more vulnerable to everything else.
Simplifying your routine is almost always the right move. The fewer products, the lower the chemical load, and the less likely that one of them is quietly destabilizing your skin.
Related: Why Over Cleaning Makes Lichen Sclerosus Worse
3. Microbiome disruption
The vaginal and vulvar microbiome, the community of microorganisms that colonize the area, plays a significant role in maintaining a stable local environment. When that balance shifts, the immune response in the skin can become more active.
The most common disruptors are antibiotics (which eliminate protective bacteria alongside pathogenic ones), recurrent yeast infections, bacterial vaginosis, and the overuse of antimicrobial products. Each of these can temporarily destabilize the microbial environment, and that instability can act as a trigger for LS flares.
This is one reason why some patients notice a clear connection between antibiotic courses and subsequent flares, sometimes appearing days to a week after the antibiotics finish, which makes the link easy to miss if you're not watching for it.
It's also worth knowing that LS patients are generally more susceptible to secondary infections, which themselves become triggers, creating a cycle where infection causes a flare, the flare makes the skin more vulnerable, and that vulnerability invites further infection.
4. Hormonal shifts
Hormones don't cause lichen sclerosus, but they profoundly influence the quality of the tissue it affects. The vulva, glans, and perianal zones are dense with hormone receptors. When hormonal balance shifts, the skin's capacity to maintain thickness, elasticity, and hydration changes with it, and that change directly affects how vulnerable it is to every other trigger on this list.
The conventional explanation focuses on estrogen: when estrogen declines, tissue thins and tears more easily. That's true, but it's incomplete, and for many LS patients, particularly around menopause, it misses the more important part of the picture.
What happens at menopause is not simply that estrogen drops. It's that progesterone collapses first and more steeply. Progesterone is the natural brake on fibrosis, it suppresses TGF-β signaling, calms mast cells, and reduces histamine driven itch. When progesterone falls faster than estrogen, the result is a state of relative estrogen dominance: not necessarily high estrogen in absolute terms, but estrogen activity that is no longer balanced by progesterone's moderating influence. This imbalance matters because excess estrogen relative to progesterone can actually drive histamine release and immune reactivity, the opposite of what you might expect if you assume estrogen is simply protective.
This helps explain a pattern many patients recognize but rarely get an explanation for: flares that don't improve with topical estrogen alone, or that seem to worsen during certain hormonal interventions. The issue often isn't estrogen deficiency per se, it's progesterone insufficiency and the resulting loss of its antifibrotic, mast cell calming effects.
The menstrual cycle tells a similar story. Patients who notice that their symptoms worsen in the week before menstruation are experiencing the luteal phase progesterone drop, the point in the cycle when progesterone, which had been rising, begins to fall sharply before the period. This drop can destabilize mast cells, increase histamine tone, and reduce the skin's resilience, all within a predictable window. Symptoms that improve after menstruation begins, when the hormonal environment resets, confirm this pattern.
Estrogen still matters. In genuinely hypoestrogenic states, deep menopause, prolonged postpartum breastfeeding, surgical menopause, the tissue can become thin, pale, and prone to fissuring in ways that look and feel similar to active LS but are partly driven by tissue atrophy rather than immune activity alone. Low dose local estrogen in these cases can improve tissue quality, though it does not suppress the underlying immune process.
Androgens are part of the picture too. Testosterone and DHEA give vulvar tissue density, thickness, and lubrication. Androgen deficiency, which accelerates with age and is common in postmenopausal women, contributes to tissue fragility and, in men with lichen sclerosus, to phimosis progression.
The full hormonal picture, testing, interpretation, and how hormonal support fits phase by phase into a management strategy, deserves its own dedicated article, which is coming. The key point here is that the hormonal trigger in LS is rarely a simple story of "estrogen low, estrogen needed." It's a question of hormonal balance, and progesterone's role in that balance is frequently the missing piece.
5. Infections
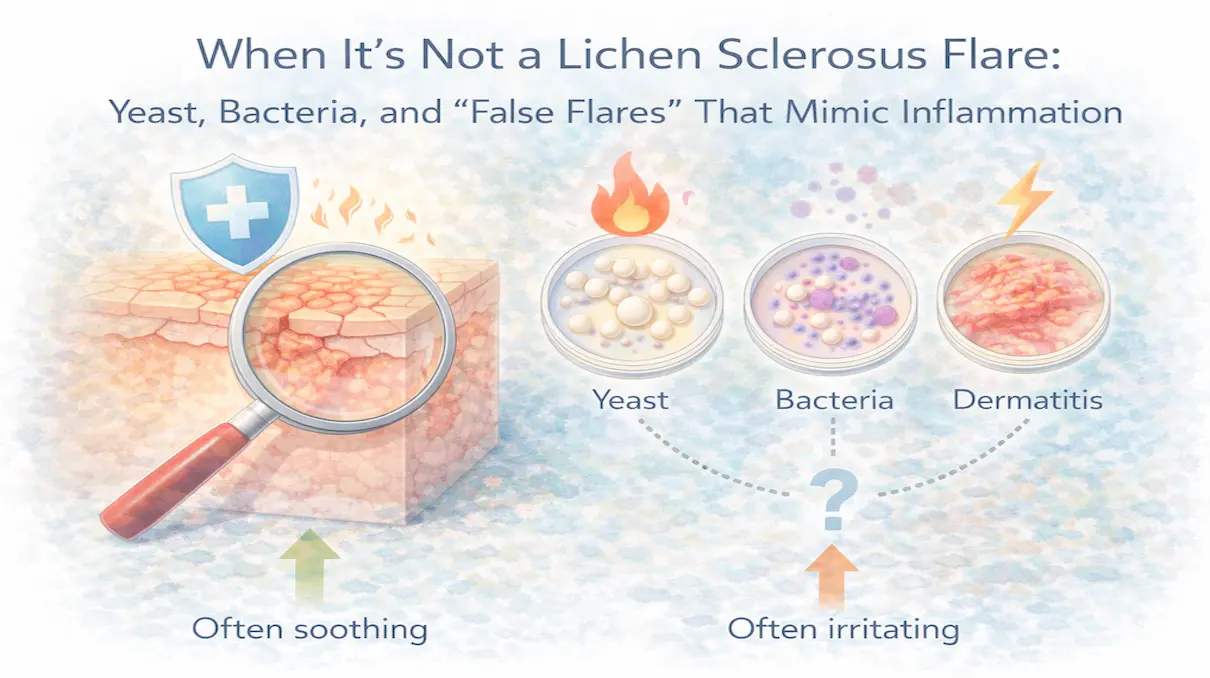
Any infection in or near the affected area can trigger or worsen a flare. Yeast infections are the most common, and because their symptoms overlap so closely with LS, patients sometimes don't realize they have both simultaneously. A positive yeast swab during a flare doesn't mean the flare is caused solely by yeast; it may mean you have two concurrent problems, each making the other worse.
Bacterial infections, urinary tract infections, and viral flares can all have a similar effect. The mechanism is the same: an infection activates immune responses in the tissue, and that immune activation spills over into the already sensitized LS skin.
When infections occur, they also tend to increase local moisture (from discharge or altered secretions), prompt more frequent washing, and sometimes require antibiotics, all of which then become secondary triggers themselves. Infections don't just cause one flare; they can start a chain.
6. Chronic low level irritation
This is the trigger category that surprises patients most: the idea that a flare can result from nothing dramatic, just small irritations accumulating over days until the skin finally tips over its threshold.
Consider what this looks like in practice. Rough toilet paper used several times a day. Residual urine that's not quite fully dried. A sanitary pad worn for too many hours. Long periods of sitting in the same position. These are not events, they're chronic background stressors. Individually, none of them would cause a problem. But stack them up day after day, and they can gradually erode the skin's resilience until a flare appears seemingly out of nowhere.
This is why the "it came out of nowhere" experience is so common. The flare didn't come from nowhere. It came from forty eight hours of accumulated low grade stress that the skin had finally had enough of.
7. Stress and metabolic strain
Psychological stress influences immune function through several pathways, including hormonal signaling (cortisol affects inflammatory response) and direct effects on immune cell behavior. Many patients notice a consistent connection between stressful periods, a difficult week at work, a family crisis, poor sleep sustained over time, and an increased frequency of flares.
Physical stressors have a similar effect: illness, surgery, significant sleep deprivation, or periods of nutritional depletion can all shift the body into a state where inflammatory responses are less well regulated.
This doesn't mean stress causes LS or that managing stress will cure it. But for patients who notice a clear connection, it's worth taking seriously as part of the overall picture.
Related: Stress, Flares, and the Nervous System: Why Lichen Sclerosus Worsens Without Visible Triggers
Why your triggers are not the same as someone else's
This point gets missed constantly in online LS communities. Someone posts that they eliminated dairy and their symptoms improved. Someone else swears by a particular oil. Another patient follows both recommendations and sees no change, or gets worse.
Trigger sensitivity is highly individual. Two patients with identical diagnoses can have completely different trigger profiles. One reacts strongly to friction but tolerates most products. Another handles friction fine but flares at the slightest change in her hygiene routine. A third has no clear pattern related to products or activity, but flares consistently around her period.
This individuality has a practical implication: copying someone else's management strategy is an unreliable approach. It might work, if your triggers happen to overlap. But just as often it won't, and the failure doesn't mean the approach was wrong in principle, just wrong for your particular pattern.
The goal is not to find the universal LS protocol. The goal is to find your protocol, based on your own observation over time.
How to identify your personal trigger pattern
You don't need a formal system. You need consistency and a willingness to pay attention for long enough that patterns become visible.
The 48 hour rule. Triggers don't always produce symptoms immediately. The skin often takes 24 to 48 hours to react. This lag is one of the main reasons triggers go unrecognized, by the time the flare appears, you're no longer thinking about what happened two days ago. When a flare starts, cast your mind back two days, not just to yesterday.
Start a simple log. It doesn't need to be elaborate. A note on your phone works. After each flare, record three things: when it started, what your symptoms were, and what was different in the 48 hours before it started. After six to eight weeks, read back through it. Patterns that were invisible day to day often become obvious when you see them across multiple entries.
Change one thing at a time. If you suspect a product is triggering flares, remove it for four weeks and observe. Don't change three things at once, you won't be able to tell which change mattered. Methodical elimination takes patience, but it actually works.
Pay attention to context, not just products. Triggers aren't only what you apply to your skin. They include what you wore, what activities you did, where you were in your menstrual cycle, how you slept, whether you were ill or stressed. The log is most useful when it captures context, not just product names.
Notice what doesn't trigger you. This is equally useful. If you've exercised six times this month and only one session was followed by a flare, friction from exercise alone probably isn't your primary trigger. Something else was different that day.
Triggers and phases: an important nuance
One thing that makes trigger identification complicated is that the same trigger doesn't always produce the same response. Something you tolerate fine during a stable period can cause a significant flare when your skin is already fragile or inflamed.
This is because LS skin moves through phases, inflammatory, erosive, fibrotic, and remission, and the threshold for triggering a flare is different in each. During a flare or a period of barrier fragility, the skin is primed for overreaction. During remission, it's more resilient. The trigger that crosses the threshold during one phase may fall short during another.
This is why consistent protective habits matter more during vulnerable phases, not because the triggers are worse, but because the skin's capacity to handle them is temporarily reduced.
Your personal trigger checklist
Lichen sclerosus trigger checklist
Review this list and mark the categories most relevant to you. Use it as a starting point for your observation log.
Friction & physical
- Tight underwear or clothing (waistbands, seams, thongs)
- Synthetic fabrics that trap heat or moisture
- Exercise involving repetitive movement or pressure (cycling, spinning, running)
- Long periods of sitting, especially on hard surfaces
- Sexual activity without adequate lubrication
- Hot weather or excessive sweating in the area
Products & chemical
- Fragranced soaps, shower gels, or feminine washes
- Wet wipes or cleansing cloths
- Scented panty liners or sanitary products
- Fabric softener or scented laundry detergent
- Bubble baths, bath bombs, or bath oils
- Topical products that cause consistent stinging or burning
Microbiome & infection
- Recent antibiotic course (flare appearing days to a week after finishing)
- Recurrent yeast infections
- Bacterial vaginosis
- Urinary tract infections
- Overuse of antimicrobial or antibacterial washes
Hormonal
- Symptoms worse in the week before menstruation
- Flares that began or worsened around menopause
- Postpartum or breastfeeding period
- Hormonal contraceptive changes
Chronic low level irritation
- Rough or fragranced toilet paper
- Residual urine irritation (incomplete drying)
- Wearing a pad or liner for extended periods
- Prolonged sitting in damp or warm clothing
Stress & metabolic
- Flares consistently following stressful periods
- Worsening during illness or physical strain
- Disrupted sleep sustained over several days
- Significant dietary changes or prolonged nutritional gaps
What to do with what you find
Identifying your triggers doesn't mean spending your life avoiding everything. That's neither possible nor the goal. The goal is to understand which factors reliably destabilize your skin, so you can make informed choices about when to be more careful.
During stable periods, your skin may handle many of these triggers without incident. During vulnerable periods, when you're in a flare, when the skin barrier is fragile, when you're going through a hormonal transition, reducing your trigger load becomes more important, because your threshold is temporarily lower.
Think of it as managing exposure, not achieving perfection. You don't have to eliminate friction from your life. You do need to know that on days when you've already exercised, worn tight clothing, and slept poorly, adding a new product to your routine is probably not the day to experiment.
The patients who manage lichen sclerosus most effectively are the ones who've moved from reacting to flares to anticipating them. That shift starts with knowing your triggers.
Related: Sex and Lichen Sclerosus: How to Reduce Friction, Pain, and Post-Sex Flares
Related: Daily Care for Lichen Sclerosus: What Helps vs What Makes It Worse
Related: Can Lichen Sclerosus Go Into Remission? What the Evidence Says
Content sourced from: Lichen Sclerosus Decoded, A New Way to Understand and Manage Lichen Sclerosus. For informational purposes only. This article does not constitute medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.